https://www.aafp.org/afp/2016/1201/p884.html
Hormone Therapy and Other Treatments for Symptoms of Menopause
The results of large clinical trials have led physicians and patients to question the safety of hormone therapy for menopause. In the past, physicians prescribed hormone therapy to improve overall health and prevent cardiac disease, as well as for symptoms
www.aafp.org
Combined estrogen/progestogen therapy, but not estrogen alone, increases the risk of breast cancer when used for more than three to five years.
Therefore, in women with a uterus, it is recommended that physicians prescribe combination therapy only to treat menopausal symptoms such as vasomotor symptoms (hot flashes) and vaginal atrophy, using the smallest effective dosage for the shortest possible duration.
Although estrogen is the most effective treatment for hot flashes, nonhormonal alternatives such as low-dose paroxetine, venlafaxine, and gabapentin are effective alternatives.
Women with a uterus who are using estrogen should also take a progestogen to reduce the risk of endometrial cancer.
Women who cannot tolerate adverse effects of progestogens may benefit from a combined formulation of estrogen and the selective estrogen receptor modulator bazedoxifene.
black cohosh, botanical products, omega-3 fatty acid supplements - not helping
One systematic review suggests modest improvement in hot flashes and vaginal dryness with soy products, and small studies suggest that clinical hypnosis significantly reduces hot flashes.
Patients with genitourinary syndrome of menopause may benefit from vaginal estrogen, nonhormonal vaginal moisturizers, or ospemifene (the only nonhormonal treatment approved by the U.S. Food and Drug Administration for dyspareunia due to menopausal atrophy).
There is no evidence that using low-dose vaginal estrogen increases the risk of breast cancer recurrence.
Risks and Benefits of Hormone Therapy
combined oral regimen consisting of conjugated equine estrogen and medroxyprogesterone with placebo, and found that the combined regimen increased the risk of coronary artery disease, breast cancer, stroke, and venous thromboembolism (VTE). The study also found a decreased risk of colorectal cancer, hip fractures, and total fractures with combined hormone therapy.
women without a uterus = those taking estrogen alone -> had no significant change in risk of coronary heart disease or breast cancer.
but increase in strokes and VTE (similar to the trial of combined estrogen and progestogen)
Estrogen - Stroke, VTE
combined hormone therapy had a significantly increased risk of breast cancer and VTE, and a reduction in hip fractures. In contrast, women taking estrogen alone had a significantly reduced risk of breast cancer.
timing hypothesis : starting hormone therapy early in menopause (compared with starting it 10 years or more after the onset of menopause) may be cardioprotective because of estrogen's apparent ability to slow the progression of atherosclerosis in younger women.
Vasomotor Symptoms : common in women with a higher body mass index, with lower income and education, who smoke cigarettes, or who are black
Estrogen is the most effective therapy for hot flashes
there is no evidence that lowering the ambient temperature; using fans; exercising; or avoiding triggers, such as alcohol and spicy foods, improves hot flashes
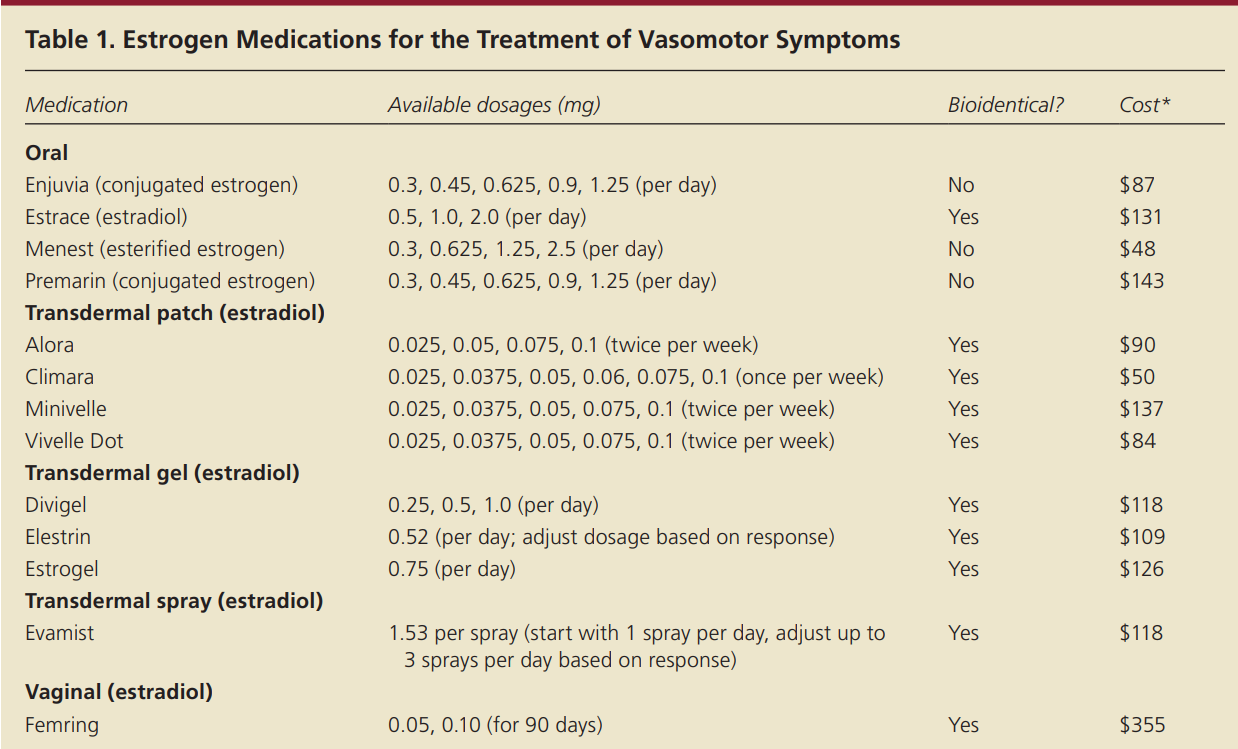
transdermal estrogen, which avoids the first-pass liver effect, may have a lower risk of VTE compared with oral estrogen
the dosage may be increased after evaluating for effectiveness during the first eight weeks of therapy, with reassessment annually or as needed.

Progestogens can cause fatigue, dysphoria, and fluid retention.
Patients with a uterus who cannot tolerate these adverse effects may benefit from Duavee, a combination of 0.45-mg conjugated equine estrogen and the selective estrogen receptor modulator bazedoxifene, which is approved by the FDA for treating hot flashes and preventing osteoporosis. Bazedoxifene does not stimulate the endometrium. Duavee is contraindicated in women who have a history of breast cancer or VTE.
The levonorgestrel-releasing intrauterine system (Mirena) is an off-label option for providing local progestogen to the endometrium for patients who cannot tolerate systemic therapy.
Low-dose paroxetine (Brisdelle) is the only nonhormonal medication approved by the FDA to treat hot flashes, Patients taking tamoxifen should not use paroxetine because of inhibition of the hepatic enzyme cytochrome P450 2D6, which decreases the effectiveness of tamoxifen. Desvenlafaxine (Khedezla) and venlafaxine do not inhibit CYP2D6 and are appropriate alternatives.
Other nonhormonal options include gabapentin (Neurontin) and pregabalin (Lyrica). These medications can cause dizziness and other adverse effects, and should be titrated from a lower dosage.

Deciding When to Discontinue Hormone Therapy
after three to five years. Clinicians should inform patients that some women will have a difficult time stopping hormone therapy.
Transitioning from Contraception to Hormone Therapy
Genitourinary Syndrome of Menopause
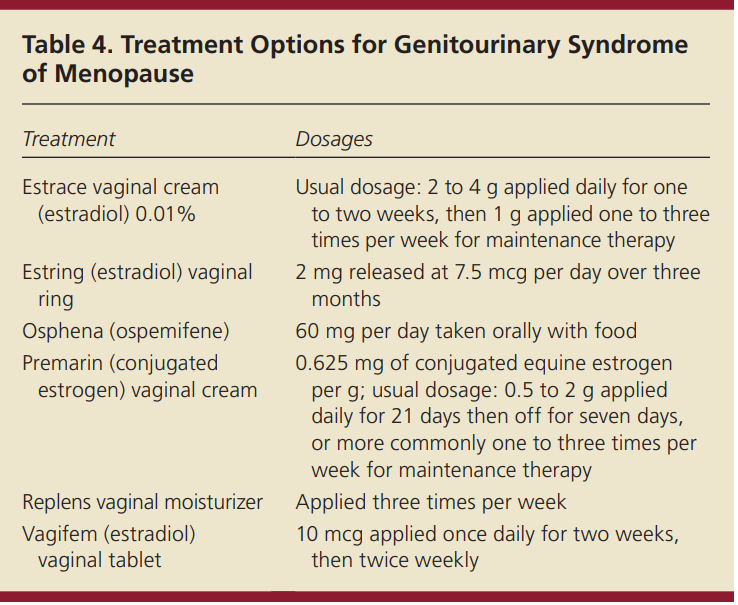
This condition affects up to one-half of women during menopause. In 2014, a consensus conference endorsed the new term genitourinary syndrome of menopause to replace the terms vulvovaginal atrophy and atrophic vaginitis, partly because the older terminology does not encompass the extent of genital tract symptoms many women experience.
Thinning of the vulvar mucosa may cause vulvar burning, irritation, or constriction of the introitus, resulting in entry dyspareunia.
vaginal estrogen, nonhormonal vaginal moisturizers, and the newer oral systemic estrogen agonist-antagonist ospemifene (Osphena). It is reasonable to try nonhormonal therapy as a first-line option to alleviate vulvovaginal symptoms caused by genitourinary syndrome of menopause.